When you decide to take the step towards better vein health, it’s essential to understand what happens during a vein doctor consultation. At Vein Doctor for Women, we prioritize your comfort and clarity throughout the process. Our team of board-certified vein doctors is here to guide you every step of the way. Here’s a detailed look at what you can expect during your appointment.
Step 1: Initial Check-In and Medical History Review
When you first arrive at our clinic, you’ll be greeted by our friendly reception staff. We’ll check you in and ask you to fill out a comprehensive medical history form. This form is crucial as it provides us with information about your past and current health status, any medications you’re taking, and any previous vein treatments you may have had. Understanding your history helps us identify any underlying conditions that may be contributing to your vein issues.
Step 2: Consultation with Your Vein Doctor
After you’ve completed your medical history form, you’ll meet with one of our board-certified vein doctors. This part of the vein doctor consultation process is vital for building a rapport and establishing a clear understanding of your concerns.
- Your doctor will ask about your symptoms, such as pain, swelling, heaviness, or visible veins.
- We’ll discuss your activities, work habits, and any factors that might affect your vein health.
- It’s important to understand what you hope to achieve from the treatment, whether it’s aesthetic improvement, pain relief, or overall better leg health.

Step 3: Physical Examination
Next, your vein doctor will conduct a thorough physical examination of your legs. This examination helps us assess the severity and extent of your vein issues. The doctor will look for visible signs of varicose veins, spider veins, or other abnormalities and feel for any irregularities in the veins using gentle pressure.
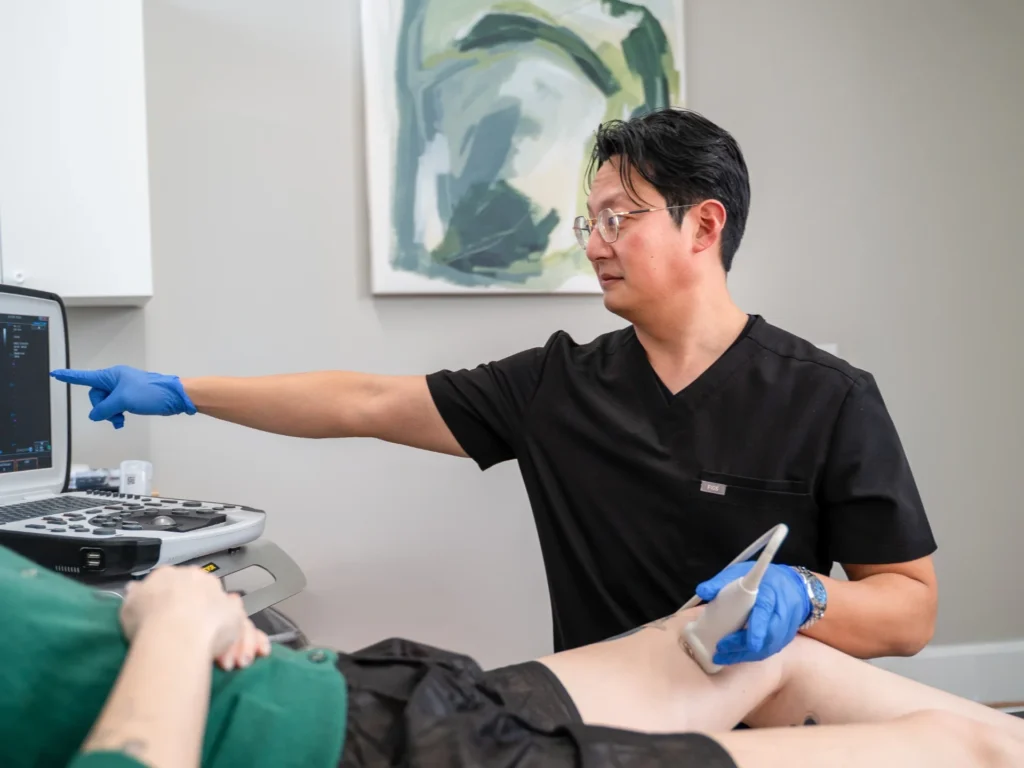
Step 4: Diagnostic Ultrasound
One of the most crucial steps in the vein doctor consultation process is the diagnostic ultrasound. This non-invasive test allows us to see inside your veins and evaluate their function. During the procedure, a special gel is applied to your legs to help transmit sound waves. The vein doctor will use a handheld device to send sound waves through your veins. These sound waves create detailed images of your veins, showing blood flow and identifying any blockages.
Step 5: Diagnosis and Discussion of Findings
After the ultrasound, your vein doctor will review the images and discuss the findings with you. This step is crucial for understanding the nature of your vein issues and planning the appropriate treatment. Based on the ultrasound results, you’ll receive a diagnosis such as chronic venous insufficiency, varicose veins, or spider veins. The doctor will explain the condition in detail, including its causes and potential complications if left untreated.
Step 6: Personalized Treatment Plan
Lifestyle Modifications
Lifestyle modifications are often the first line of defense in managing vein issues and improving overall vein health. These changes can significantly reduce symptoms and prevent further deterioration of your veins. Here are some detailed recommendations:
- Compression Stockings: Compression stockings apply pressure to your legs, helping to improve blood flow and reduce swelling. There are various types of compression stockings, ranging from mild to strong compression. Your doctor will recommend the appropriate level based on your condition. It’s essential to wear them as prescribed, typically during the day when you are most active. They should be put on in the morning and taken off before bed.
- Leg Elevation: Elevating your legs above heart level helps reduce venous pressure and swelling. You should elevate your legs several times a day for 15-20 minutes each time. When resting or sleeping, consider using pillows to keep your legs elevated. Regular elevation can help alleviate symptoms like swelling and discomfort by reducing fluid buildup.
- Regular Exercise: Physical activity is crucial for promoting healthy blood circulation. Exercise helps the calf muscles act as a pump, aiding in blood flow back to the heart. Low-impact exercises like walking, cycling, and swimming are particularly beneficial. Aim for at least 30 minutes of moderate exercise most days of the week.
Minimally Invasive Procedures
For many patients, minimally invasive procedures are an effective way to treat vein issues with minimal downtime and discomfort. These procedures are performed on an outpatient basis and typically allow you to return to your normal activities quickly. Here are some of the most common minimally invasive vein treatments:
- Sclerotherapy: A solution, often a saline or a detergent-based substance, is injected directly into the affected veins. This solution irritates the lining of the veins, causing them to collapse and eventually be reabsorbed by the body. Sclerotherapy is commonly used for treating spider veins and smaller varicose veins.
- Endovenous Laser Treatment (EVLT): EVLT involves inserting a small laser fiber into the affected vein through a tiny incision. The laser emits energy that heats and seals the vein, causing it to collapse and be reabsorbed by the body. EVLT is effective for treating larger varicose veins and chronic venous insufficiency.
- Radiofrequency Ablation (RFA): Similar to EVLT, RFA uses radiofrequency energy instead of laser energy to heat and close the affected vein. A catheter is inserted into the vein, and radiofrequency energy is delivered to seal the vein shut. RFA is suitable for large varicose veins and is particularly effective for patients with venous reflux disease.
- Ambulatory Phlebectomy: This procedure involves removing varicose veins through small, minimally invasive incisions. A special hook is used to extract the vein in sections. It is ideal for bulging varicose veins close to the skin’s surface.
Step 7: Discussion of Risks and Benefits
Before proceeding with any treatment, it’s essential to understand the risks and benefits. Your vein doctor will provide a comprehensive overview to help you make an informed decision. The benefits might include improved appearance, reduced pain and swelling, and better overall leg health. Potential risks, although minimal with minimally invasive procedures, will be discussed, such as infection, bruising, or allergic reactions.
Step 8: Scheduling and Next Steps
Once you’ve agreed on a treatment plan, we’ll help you schedule your procedures and follow-up appointments. This ensures you know what to expect moving forward and can plan accordingly. We’ll schedule dates for any planned treatments. Regular follow-ups are essential to monitor your progress and make any necessary adjustments to your treatment plan.
Step 9: Pre-Procedure Instructions
If your treatment includes a procedure, we’ll provide detailed pre-procedure instructions. Following these guidelines helps ensure the best possible outcome. Instructions may include:
- Guidance on which medications to avoid before your procedure.
- Information on whether you need to fast prior to treatment.
- Recommendations on what to wear for comfort and convenience.
Step 10: The Procedure Day
On the day of your procedure, you will receive all the support you need to feel comfortable. We’ll prepare you for the procedure, including cleaning the treatment area and applying any necessary anesthetic. Your vein doctor will perform the treatment, explaining each step as they go. Post-procedure care instructions will be provided to ensure a smooth recovery.
Step 11: Post-Procedure Care and Follow-Up
After your procedure, proper care and follow-up are crucial for achieving the best results. We’ll provide you with detailed post-procedure instructions and schedule follow-up visits to monitor your progress. We’ll advise on any activity restrictions to promote healing and describe which symptoms are normal and which require immediate attention.
Initiate Your Vein Doctor Consultation Process
The vein doctor consultation process at Vein Doctor for Women is thorough, informative, and tailored to your unique needs. Our goal is to ensure you feel supported and informed every step of the way. By understanding what to expect during your appointment, you can approach your consultation with confidence. If you have any questions or are ready to schedule your consultation, please don’t hesitate to contact us.